- (318) 933-DERM (3376)
- Info@Cenladerm.com
- Monday - Thursday 8:00AM - 5:00PM - Friday 8:00AM - 01:00PM
- (318) 933-DERM (3376)
- Info@Cenladerm.com
-
Monday - Thursday 8:00AM - 5:00PM
Friday 8:00AM - 01:00PM
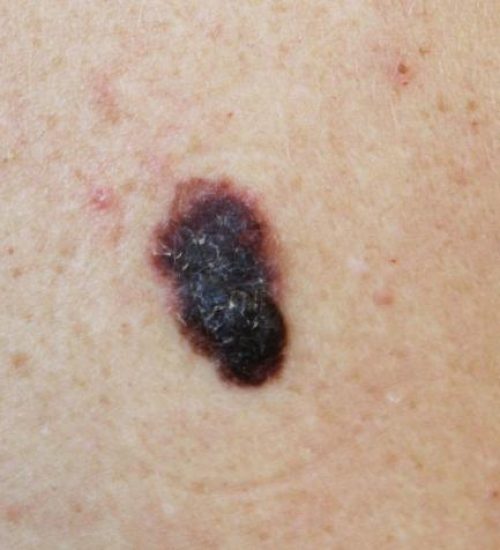
Skin cancer is the most common form of cancer in the United States. There are more cases of skin cancer in the U.S. than breast, colon, and lung cancer combined. Most skin cancers are caused by ultraviolet (UV) exposure, including: intense intermittent sun exposure, multiple sunburns, long-term cumulative sun exposure over many years, or through tanning bed use. While skin cancer is more common in lighter skin (those with green or blue eyes and lighter hair), it can occur in skin of every color.
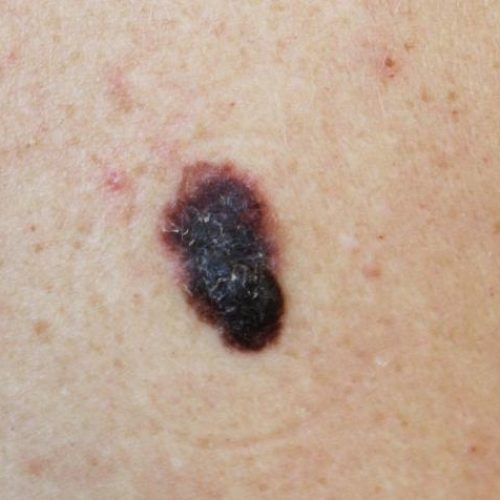
Skin cancer is the most common form of cancer in the United States. There are more cases of skin cancer in the U.S. than breast, colon, and lung cancer combined. Most skin cancers are caused by ultraviolet (UV) exposure, including: intense intermittent sun exposure, multiple sunburns, long-term cumulative sun exposure over many years, or through tanning bed use. While skin cancer is more common in lighter skin (those with green or blue eyes and lighter hair), it can occur in skin of every color.
An important part of our job as dermatology-trained healthcare providers is early detection of skin cancer. Fortunately, with early detection, most skin cancers are treatable. We encourage our patients to perform self-examinations of their skin frequently, bring suspicious lesions to our attention, and come in for a full-body skin examination annually. After diagnosis with a skin cancer, you are more likely to develop another skin cancer. Therefore, you may need more frequent full-skin examinations by a dermatologist to survey the skin for new or recurrent skin cancers after one skin cancer diagnosis. In addition, continued sun protection and sunscreen use are necessary measures to decrease the development of new skin cancers.
Basal Cell Carcinoma (BCC)
Basal cell carcinoma (BCC) is the most common form of skin cancer. A BCC can have many appearances, but most commonly it appears as a slightly shiny, pink, flesh-colored, or red bump. BCC may appear pimple-like initially, but, unlike a pimple, it does not heal after 3-4 weeks. BCC may also appear as a red scaly rash-like patch, a scar, or a small sore that bleeds easily. Common locations for BCC are the scalp, face, ears, neck, chest, arms, hands, and legs. Basal cell carcinoma has a low rate of metastasis, or spread to other places in the body, but it can be destructive to the area affected by the tumor, including cartilage and bone. When caught early, BCCs respond well to treatment.
Treatment options for BCC include surgical and skin-based therapies. Surgical excision, Mohs micrographic surgery, and electrodessication and curettage (scraping and burning the abnormal tissue) are the most common forms of treatment. Photodynamic therapy (PDT) and prescription topical creams like 5-fluorouracil or imiquimod cream may be used to treat superficial basal cell carcinomas. Radiation therapy and cryotherapy (freezing) are occasionally used depending on the patient.
Squamous Cell Carcinoma (SCC)
Squamous cell carcinoma (SCC) is the second most common form of skin cancer. At least 40-60% of squamous cell carcinomas can be traced back to a previously existing precancerous lesion, called an actinic keratosis. SCCs usually present as red scaly, sometimes tender spots that are growing in size or that do not respond to treatment as a pre-cancer would. They can also present as a non-healing sore or a wart-like spot. At times, SCCs may be irritated or painful. SCCs occur on the scalp, face, ears, lips, neck, arms, hands, and legs but can also occur on mucous membranes and the genital area. Additionally, they may develop in burn scars or non-healing ulcers. SCCs have a greater risk of spread, or metastasis, than basal cell carcinomas do, with 5-10% of SCCs metastasizing to other organs. SCCs on the lips are at greatest risk of spread. According to the Skin Cancer Foundation, 2,500 deaths each year are due to squamous cell carcinoma of the skin.
Surgical excision and Mohs micrographic surgery are the most common treatments for squamous cell carcinoma. Electrodessication and curettage (scraping and burning the tissue) may also be used depending on the location and the specific patient. Photodynamic therapy (PDT), radiation therapy and cryotherapy (freezing) are occasionally used depending on the patient. Prescription topical treatments like 5-fluorouracil or imiquimod cream may be used before, during, or after treatment of squamous cell carcinoma.
Skin cancer treatment with Mohs micrographic surgery
Mohs is a skin-sparing surgical technique developed in the 1930’s that allows for 100% microscopic examination of the surgical margin to ensure all of the cancerous tissue is removed during the surgery. The main advantage of Mohs micrographic surgery is its complete examination of the tissue margin. Some skin cancers are larger than anticipated, or have “roots” that may be missed if simple surgical excision with standard margins is performed. The Mohs procedure has a 99% cure rate for non-melanoma skin cancers, but is reserved for specific clinical presentations of skin cancer: those located on the face or scalp, large lesions on the body, recurrent skin cancers, and aggressive types. The Mohs surgical procedure and repair is usually performed on the same day and completed in-office under local anesthesia.
Mohs micrographic surgery is a specialized in-office surgery for skin cancers. Dermatologists who perform Mohs micrographic surgery have specialized residency, fellowship, or other intensive training experience. These dermatologic surgeons have appropriate laboratory facilities and equipment that allows them to examine the excised tissue on the same day as the surgery.
The dermatologists at Cenla Dermatology do NOT perform Mohs skin surgery. However, if you are diagnosed with a skin cancer, our highly educated providers can help you determine whether or not you need Mohs and refer you to a Mohs trained provider if so. Our providers can also help with scar improvement once the Mohs procedure is complete.